The Difference Between Perimenopause and Menopause
A UK Guide to Understanding the Stages, Symptoms, and What to Expect
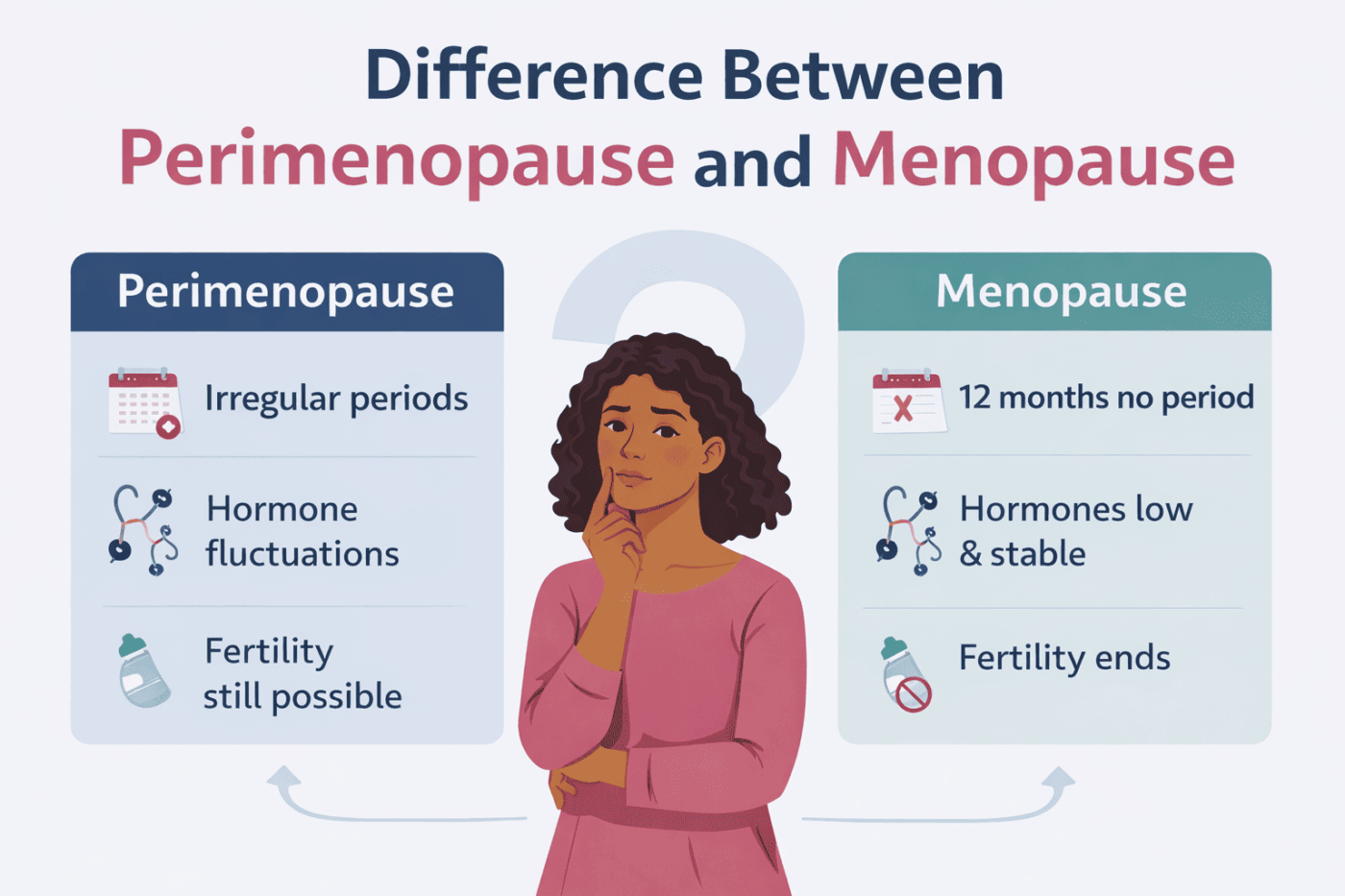
| Quick Answer: Perimenopause vs Menopause • Perimenopause is the transitional phase before menopause, where hormones fluctuate and periods become irregular • Menopause is confirmed after 12 consecutive months without a period • Perimenopause can last several years; menopause is a single point in time • Both stages are a normal part of life, and both deserve proper support |
Introduction
For many women, the confusion doesn’t come from symptoms, it comes from not knowing what to call what’s happening.
If you’ve ever used ‘perimenopause’ and ‘menopause’ as though they mean the same thing, you’re far from alone. But understanding the difference between perimenopause and menopause can help you get the right diagnosis, explore the right treatments, and set realistic expectations for what lies ahead.
Whether you’re experiencing new symptoms and wondering what’s happening to your body, trying to understand a recent GP conversation, or simply planning ahead – this guide is for you.
In this UK guide, we explain what perimenopause and menopause are, how they differ, when they typically begin in the UK, and what you can do to manage your wellbeing throughout this natural – and very normal – phase of life.
What Is Perimenopause?
If you are searching what is perimenopause UK, here is a clear answer: perimenopause is the transitional phase that leads up to menopause. The word itself means ‘around menopause’, and it describes the years during which your body begins producing less oestrogen and progesterone in preparation for the end of your menstrual cycle.
What Happens to Your Hormones?
During perimenopause, oestrogen and progesterone don’t decline in a smooth, predictable line – they fluctuate. Some months oestrogen may spike; others it drops sharply. This hormonal instability is the root cause of most perimenopause symptoms, and it’s why the experience can feel so erratic and hard to pin down.
Why Symptoms Feel Unpredictable
Because hormone levels are rising and falling rather than simply declining, symptoms during perimenopause can vary enormously from week to week. One week you might feel completely like yourself; the next you’re drenched in sweat at 3am, foggy-headed, and tearful without knowing why.
Perimenopause typically lasts between four and ten years, though for some women it can be shorter. It ends when you’ve gone 12 consecutive months without a period – at which point you’ve reached menopause.
Throughout this phase, your periods become irregular but haven’t stopped completely. You might experience:
- Cycles that are shorter or longer than usual
- Heavier or lighter bleeding than you’re accustomed to
- Skipped periods followed by a return of your cycle
What Is Menopause?
Menopause is not a long phase – it is a single point in time. Specifically, it is the moment 12 consecutive months have passed without a menstrual period, confirming that your ovaries have stopped releasing eggs and your reproductive hormones remain at a consistently lower level.
Many women ask when does menopause start in the UK. The average age of menopause in the UK is 51, though it can occur naturally anywhere between the mid-forties and mid-fifties.
After that 12-month milestone, you enter postmenopause. Many people refer to the years following menopause simply as ‘menopause’, which adds to the confusion – but technically, the word refers only to that defined threshold moment.
Once menopause has occurred:
- Your periods have permanently stopped
- Hormone levels are low and stable (rather than fluctuating)
- Natural pregnancy is no longer possible
Perimenopause vs Menopause: Key Differences Explained
The question of perimenopause vs menopause UK comes down to a few fundamental distinctions. The table below summarises them clearly:
| Feature | Perimenopause | Menopause |
| Periods | Irregular – lighter, heavier, or skipped | Stopped for 12+ consecutive months |
| Hormones | Fluctuating – oestrogen & progesterone declining unevenly | Consistently low and stable |
| Symptoms | Unpredictable – can vary week to week | May stabilise, but can still be significant |
| Fertility | Reduced but still possible | Natural pregnancy is no longer possible |
| Duration | Typically 4–10 years | A single point in time (then postmenopause) |
| Diagnosis | Based on symptoms and age | Confirmed after 12 months without a period |
How Do I Know If I Have Perimenopause or Menopause?
This is one of the most common questions women bring to their GP – and the answer can feel frustratingly unclear at first.
Why Diagnosis Can Feel Confusing
In the UK, perimenopause is typically diagnosed based on your symptoms and age rather than blood tests alone. If you are over 45 and experiencing new or changed symptoms alongside irregular periods, a GP should be able to diagnose perimenopause clinically – without necessarily running hormone tests.
Common signs that suggest you may be in perimenopause include:
- Periods becoming irregular, heavier, lighter, or more infrequent
- Hot flushes or night sweats appearing for the first time
- Changes in mood, sleep, or energy levels that feel out of character
- Vaginal dryness or changes in sexual function
Confirming Menopause
Menopause is confirmed retrospectively – once 12 consecutive months have passed without a period. At that point, there is no ambiguity. You don’t need a blood test to confirm it; the 12-month rule is the clinical standard.
A Note on Younger Women
If you are under 45 and experiencing symptoms, your GP may recommend blood tests – specifically FSH (follicle-stimulating hormone) – to investigate further. Symptoms in younger women can indicate early menopause or premature ovarian insufficiency (POI), which requires different management and warrants specialist referral.
If your symptoms are affecting your quality of life and you don’t feel listened to, you have every right to advocate for yourself or seek a second opinion.
What Is the Normal Age for Perimenopause to Begin?
Most women begin perimenopause in their mid-to-late forties, though it can start as early as the late thirties. There is no single ‘normal’ – your timeline will be influenced by genetics, lifestyle, and medical history.
Factors that can influence when perimenopause begins include:
- Family history – when your mother and sisters went through menopause is often a reasonable guide
- Smoking – associated with an earlier menopause
- Certain cancer treatments – chemotherapy and radiotherapy can trigger early or premature menopause
- Surgical menopause – removal of both ovaries causes an immediate menopause, regardless of age
- Premature ovarian insufficiency (POI) – affects roughly 1 in 100 women under 40 in the UK
Why does awareness in your thirties matter? Because perimenopause can begin earlier than most women expect, and symptoms are frequently misdiagnosed as anxiety, depression, thyroid issues, or simply stress. Knowing the signs means you’re more likely to seek support earlier and avoid years of unnecessary suffering.
Are Menopause Symptoms Worse Than Perimenopause?
Not necessarily – but they are different, and the experience varies enormously from one woman to the next.
Perimenopause tends to be the more turbulent phase, precisely because hormone levels are fluctuating rather than simply low. The unpredictability – both of your cycle and your symptoms – can make it particularly challenging to manage day-to-day life.
During menopause and into postmenopause, hormone levels stabilise at a lower level. For some women, this actually brings a degree of relief – the rollercoaster calms down. For others, symptoms such as hot flushes, vaginal dryness, and sleep disruption continue well into postmenopause.
| 💡 Key insight: There is no universal experience. Some women sail through both stages with minimal disruption. Others find perimenopause or postmenopause deeply difficult. Neither is more valid than the other, and both deserve proper support. |
What Is the Biggest Symptom of Menopause?
There is no single ‘biggest’ symptom, and framing it that way can actually be unhelpful, because it leads many women to dismiss their own experience if it doesn’t match the stereotype.
That said, the most commonly reported symptoms across both perimenopause and menopause include:
- Hot flushes – sudden waves of heat, typically affecting the face, neck, and chest
- Night sweats – hot flushes occurring during sleep, often leading to waking and disrupted rest
- Sleep disruption – difficulty falling asleep, staying asleep, or feeling rested
- Brain fog – difficulty concentrating, remembering words, or thinking clearly
- Anxiety and low mood – sometimes the first and most distressing symptoms, frequently misattributed to other causes
- Joint aches and muscle pain – less commonly discussed but widely reported
- Palpitations – a racing or irregular heartbeat, particularly associated with hormonal fluctuations
It is also worth noting that menopause symptoms are not purely physical. Changes in mood, confidence, identity, and relationships are equally real and equally deserving of attention.
Common Symptoms Across Both Stages
Although perimenopause and menopause are distinct stages, there is significant overlap in the symptoms experienced. The following are commonly reported across both:
| Shared symptoms of perimenopause and menopause: • Hot flushes and night sweats • Fatigue and disrupted sleep • Low mood, anxiety, or irritability • Brain fog and difficulty concentrating • Vaginal dryness and discomfort • Reduced libido • Changes in weight or body shape • Hair thinning or changes in skin texture |
The key distinction is not which symptoms occur, but how they present. In perimenopause, symptoms tend to fluctuate and feel erratic. In postmenopause, they are often more consistent – though they can still be significant.
When Should You Seek Support?
You don’t need to be suffering significantly before reaching out. Ideally, you’d speak to a GP or menopause specialist whenever your symptoms are affecting your quality of life – whether that means work, relationships, sleep, or your sense of self.
You should consider seeking support if:
- Your symptoms are disrupting daily life, work, or relationships
- You’re unsure whether what you’re experiencing is hormonal
- You are under 45 and experiencing any of the symptoms described above
- Your periods have stopped suddenly or unexpectedly
- You’ve been told it’s ‘just stress’ or ‘just anxiety’ and you suspect otherwise
Advocacy matters here. UK women have historically been undertreated for menopause-related symptoms, and awareness is only now catching up. If you don’t feel heard by your GP, you are entitled to ask for a referral to a menopause specialist, or to find menopause specialists, nutritionists, and therapists through our UK directory at https://themenopausedirectory.co.uk/
How to Manage Symptoms
There is no single approach to managing perimenopause and menopause – the right combination of support will depend on your symptoms, health history, and personal preferences. Most women benefit from a blend of lifestyle, medical, and holistic support.
Lifestyle Support
- Nutrition: A diet rich in phytoestrogens (flaxseeds, soya, wholegrains), calcium, and anti-inflammatory foods can support hormonal balance and bone health
- Movement: Regular exercise – including both cardiovascular activity and strength training – supports mood, sleep, bone density, and weight management
- Sleep: Prioritising sleep hygiene, managing night sweats with breathable bedding, and establishing a wind-down routine can make a significant difference to wellbeing
Medical Options
According to NICE guidelines in the UK, HRT (Hormone Replacement Therapy) is considered the most effective treatment for most menopause symptoms, and for most women the benefits outweigh the risks. It is available on the NHS and can be discussed with your GP or a menopause specialist.
- Non-hormonal medications: Options such as SSRIs, SNRIs, and clonidine can be effective for hot flushes and mood symptoms in women who cannot or prefer not to take HRT
- Local oestrogen: Vaginal oestrogen is available for genitourinary symptoms and carries minimal systemic risk
Holistic Support
- Therapy and counselling: CBT (Cognitive Behavioural Therapy) has strong evidence for reducing hot flush distress and managing anxiety related to menopause
- Menopause coaching: A growing number of specialists help women navigate this transition – particularly around identity, confidence, and lifestyle
- Community and peer support: Connecting with other women going through the same experience can reduce isolation and provide practical insight
Finding the Right Support
Despite the progress made in recent years, many women still struggle to find the right help – whether that’s a menopause-informed GP, a specialist dietitian, or a therapist who understands the emotional dimension of this transition.
Awareness of menopause varies widely across healthcare and wellness professions. A GP without specialist training may not feel confident prescribing or adjusting HRT. A personal trainer without menopause knowledge may give advice that isn’t appropriate for this phase of life.
This is exactly why we created The Menopause Directory.
| 🌿 The Menopause Directory connects you with menopause specialists, nutritionists, fitness experts, and support services across the UK – all in one place. Whether you’re looking for a menopause-aware GP, a holistic therapist, a certified nutritionist, or a women’s health coach, our directory makes it easy to find vetted professionals who truly understand this phase of life. Don’t navigate this alone. Explore trusted menopause support at The Menopause Directory today. |
In Summary
Perimenopause and menopause are related but distinct, and understanding the difference is one of the most empowering things you can do for your health.
- Perimenopause is a transition – a phase of hormonal change that can last several years, during which your periods become irregular and symptoms fluctuate
- Menopause is a defined milestone – the point at which 12 consecutive months have passed without a period
- Postmenopause follows – when hormone levels stabilise and, for many women, symptoms begin to settle
Wherever you are in this journey, you are not alone. Millions of women in the UK are navigating the same questions, the same confusing symptoms, and the same frustration at not always being taken seriously.
Understanding your body is the first step. The next is finding the right support, and we’re here to help you do exactly that.
Your trusted UK directory for menopause and wellbeing support

